Non-Communicable Diseases Get Attention
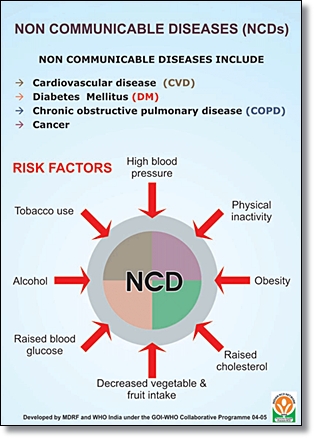 |
Non-communicable diseases such as diabetes, high blood pressure, renal disease (often secondary to the former two diseases) and chronic respiratory diseases are predominantly the result of poor (Western) lifestyle choices, often ‘imported’ to Africa by way of colonialism and economic progress. Diets high in sugar, cholesterol and fat, as well as widespread smoking and alcoholism at a young age are among the major lifestyle causes of NCDs.
Thus, there is no doubt that appropriate healthcare prevention and preventive personal behaviour can limit the number of new patients in nearly every medical category of NCDs, or, at least, reduce the costs for treatment considerably. Early diagnosis of a developing NCD can be treated with less expensive and less amount of drugs, less extensive surgery with less expensive follow-up care, and thus, overall, a significantly less burden on both the patient’s life and productivity, as well as on the country’s healthcare expenses.
While these statements are correct and can easily be voiced, the problem is that they often cannot be put into real Dollars, Euros or Rand that have been saved by promoting prevention. It is easy to summarize the costs for treatment ‘to keep a chronic ill patient relatively healthy’, or the costs of successful treatment of a specific disease; however, it is nearly impossible to put an exact value on the amount of money saved for not having to treat an x-number of people for a disease they did not develop because of preventive, sanitary, hygienic or other reasons. A rough amount of savings can only be obtained after a long-term implementation of those preventive measures by roughly comparing the overall healthcare expenses prior to the introduction of prevention with the overall expenses a few years later, adjusted for all other expense-related circumstances.
Certain preventive measures have proven to be valid and worth its costs – such as the Pap-smear for the detection of early cell changes, preventing the development of cervical cancer, still the primary cause of cancer in women almost everywhere in the world. Regular mammography for the detection of breast cancer has undoubtedly its advantages, but is cost-intensive, not widely available outside the developed world, and has recently even been questioned as to the required frequency of conducting this test. Another cost-effective and beneficial preventive measurement is undoubtedly the colonsocopy, if available and done at the right age.
The cheapest way of prevention, however, appears to be the proper education of the population about the diseases, what these diseases are, how they develop and express themselves, i.e. their early symptoms, and, of course, how to prevent getting sick in the first place. For example, educating a woman to properly and regularly perform breast self-examinations is easier to achieve and much cheaper than regular mammograms and has also shown to have a long-term beneficial effect on the early detection of breast tumors.
Fortunately, there are already a few small non-profit organizations which have spend their usually modest funds (as compared to major governmental organizations) by making an early impact on the communities in which they work and that are most affected and/or endangered by NCDs. These entrepreneurial organizations have not only recognized that the best prevention against illness is a proper education regarding the disease itself, its lifestyle causes, early symptoms and ways on how to prevent getting sick in the first place, they have also taken successful steps in implementing ‘Prevention Education.’
Unfortunately, many African governments have not yet fully recognized the importance and impact these organizations have already made and could make in the future and thus, still do not support these small organizations in the same manner as they court big governmental organizations.
‘Knowledge is the Foundation for Prevention’ [of (non-)communicable diseases]! This is a valid approach not only for preventing the spread of NCDs, but also communicable diseases such as sexually transmitted infections (STI) and especially HIV, as well as cholera or respiratory infections among many others.
We have seen that grassroots level medical and healthcare education to urban and rural communities in form of workshops, lectures and simple brochures is not only highly desired by the targeted population, it has also shown to have a profound and often immediately recognizable positive effect on the community’s healthcare behaviour.
According to the ‘Universal Declaration of Human Rights’ issued by the United Nations (UN) in 1998, at the occasion of its 50th birthday, Article 26 specifies that ‘everyone has the right to education’, which ‘shall be free in its elementary and fundamental stages.’ Certainly, the right to get to know one’s own health status, how to protect it, and how to stay healthy, would fall under the heading of ‘elementary and fundamental’ knowledge of life. Education is also the cornerstone of social and economic development of any country, setting the foundation for future well-being and prosperity. An increased awareness of a healthy lifestyle and knowledge of how to protect oneself effectively from becoming the victim of widespread diseases and illnesses has long been acknowledged and known in the medical society, as being one of the best and most efficient ways of conducting ‘prevention’.
Only a healthy person can work, create and support his/her family, consume and pay taxes, and thus become the foundation of an economically healthy country, which ultimately will not have to rely anymore on hand-outs from other countries and foreign donors.
In summary, smaller, more cost effective and efficient organizations should not be disregarded but rather courted and supported by both national and local governments.
By Dr. Tom C. Garven
Founder and Executive Director, Medicine for Africa http://www.medicinemd.com/
